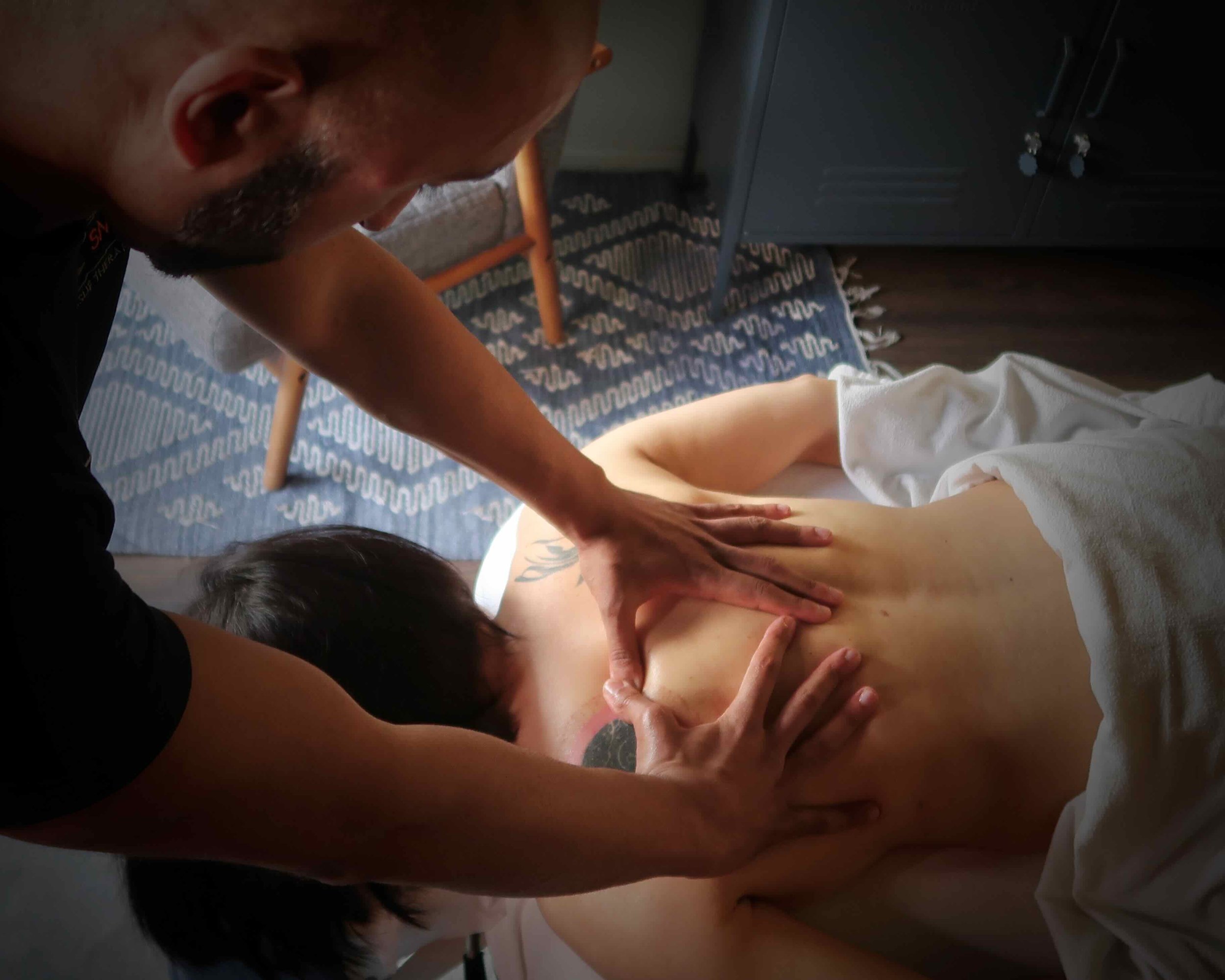
Why Massage Might Be the Missing Piece in Your Self-Care Routine
When exercise, sleep and nutrition aren’t happening - and you need a reset
By Natalie Heng, Clinical & Sports Massage Therapist (BTEC 6, SMA Reg) | Ex-Science Writer | BSc (Hons) Biology, Imperial College London
We’ve all heard the advice. Exercise regularly. Sleep well. Eat better. And it’s true - those three pillars really are the foundation of staying well and keeping pain at bay. The research backs it up, and so does clinical experience. But here’s the thing, sometimes it’s just not that simple.
Work gets intense, the commute drains you. The kids need you. Your schedule fills up. You skip the gym for a week, then two. You grab lunch at your desk. You’re too wired to sleep properly, and too tired to do anything about it. Before you know it, your neck is stiff, your shoulders are up by your ears, your lower back aches after a day of sitting, and you can’t remember the last time you felt genuinely rested.
It’s not a lack of willpower - life gets hectic for all of us sometimes. And the frustrating part? Once you’re in that state; stressed, sore, sleeping badly - it becomes harder to get back to the things you know would help.The aches make it harder to exercise. The poor sleep makes everything feel heavier. The tension feeds into anxiety, which feeds into more tension, which feeds into worse sleep. It becomes a loop.
KEY TAKEAWAYS
Stress, poor sleep and musculoskeletal pain are deeply interconnected - each one amplifies the others.
Massage may support a shift toward parasympathetic nervous system dominance, reducing cortisol and lowering resting muscle tone.
A single 30-minute session has been shown to measurably improve sleep quality indicators in poor sleepers (Ntoumas et al., 2025).
The quality of the therapeutic relationship matters. Evidence shows a strong therapeutic alliance measurably reduces pain intensity (Fuentes et al., 2014).
The Pain–Stress–Sleep Cycle
This isn’t just anecdotal. Research consistently shows that musculoskeletal pain, psychological stress, and poor sleep are deeply interconnected - each one amplifying the others.
A 2021 review in The Lancet described chronic pain as a multidimensional experience shaped not just by tissue injury but by stress, mood, sleep quality, and how safe and supported someone feels (Cohen, Vase & Hooten, 2021). The biopsychosocial model of pain - now the dominant framework in modern pain science - recognises that what’s happening in your body can’t be separated from what’s happening in your life (Moseley & Butler, 2015).
In practical terms: if you’re overworked, under-slept, and carrying chronic tension in your neck and shoulders from ten-hour days at a laptop, that pain isn’t just “mechanical.” It’s being driven, and sustained, by the stress, the fatigue, and the lack of recovery time. And simply telling someone in that state to “exercise more and sleep better” isn’t always helpful, because the pain and exhaustion are the very things standing in the way.
This is where massage can really help.
What Massage Actually Does in This Situation
Massage isn’t a magic fix, and any honest therapist will tell you that. But when someone is caught in that cycle of tension, stress, poor sleep, and pain, a skilled massage session can act as a genuine reset.
The muscle mechanics - for those who want to go deeper
Why Desk Work Specifically, Often Creates This Pattern
The upper trapezius and levator scapulae are responsible for supporting the weight of your head and stabilising your shoulders.
In an ideal world they share that load with the deep cervical flexors (longus capitis and longus colli) at the front of the neck, and the mid-back muscles behind.
But sustained desk posture - the combination of a slightly forward head position, elevated and rounded shoulders, and arms reaching toward a keyboard - tends to shift the load disproportionately onto the trapezius and levator muscles, while the deep cervical flexors - small muscles tucked along the front of your spine, behind your throat, whose job is to hold your head in position with precision - become progressively underactive.
I’ve experienced it many times myself, sitting at a desk, a couch, a not-ideal coffee table; trying to get work done on a deadline, forgetting to move for hours, and then wondering why my shoulders are aching and I feel a headache coming on.
Research using electromyography has confirmed that people with neck pain show significantly reduced activation of the deep cervical flexor muscles, with compensatory overactivity in the more superficial neck muscles - the sternocleidomastoid and anterior scalenes - which are not designed for sustained postural work (Falla, Jull & Hodges, 2004). Whether this imbalance precedes pain or develops in response to it, or both, is still being studied, but the pattern itself is well replicated and clinically consistent.
The result is a system out of balance: the wrong muscles doing too much, the right muscles contributing less than they should, and the fine postural control of the cervical spine gradually deteriorating as a consequence.
Classic upper trapezius trigger points, for instance, often refer pain up the side of the neck and into the head - which is one reason tension headaches are so common in desk workers. The headache feels like it's in the head, but the source is frequently in the shoulder.
This is also why simply resting or taking time off often doesn't fully resolve the tension. The pattern is held in place by both the physical loading and the nervous system state simultaneously - which is the subject of the section above.
Here’s what’s happening:
It reduces physical tension directly. Sustained desk postures - hunched shoulders, forward head position, static loading of the upper trapezius and levator scapulae - create patterns of muscular hypertonicity and trigger points. Hands-on soft tissue work can help reduce that tone, ease trigger point referral, and restore a sense of physical comfort. A systematic review of 26 trials found massage reduces pain and improves physical function in people with musculoskeletal conditions compared to no treatment (Bervoets et al., 2015).
It calms the nervous system. Massage has been shown to shift the autonomic nervous system towards parasympathetic (“rest and digest”) dominance - lowering heart rate, reducing sympathetic arousal, and creating a physiological state more conducive to relaxation and sleep(Diego & Field, 2009). It’s not just about the muscles. It’s about helping your whole system downregulate after weeks or months of running on stress.
It can improve sleep quality. A recent randomised controlled trial found that a single 30-minute session of either relaxation or sports massage reduced muscle tone, increased subjective relaxation, and improved indicators of sleep quality in poor sleepers (Ntoumas et al., 2025).
It gives you space to feel heard. This one often gets overlooked in the research, but it matters. A good therapist listens. They ask about your week, your pain, what’s going on. They tailor the treatment. That therapeutic alliance - the feeling of being understood and responded to - is itself a component of effective pain management. One controlled study found that an enhanced therapeutic alliance between therapist and patient significantly modulated pain intensity in people with chronic low back pain (Fuentes et al., 2014). When someone actually pays attention to how your body feels and adapts what they’re doing accordingly, it’s easier to let go. And that matters for recovery.
The Gap Massage Fills
So here’s the honest framing: massage isn’t a replacement for exercise, sleep, and nutrition. Those things remain fundamental. But massage can fill the gap when life has knocked those habits out from under you.
Think of it as a reset point. You come in carrying weeks of accumulated tension, poor sleep, and low-grade stress. A good session can bring down the physical tension, calm the nervous system, ease the aches, and help you sleep better, even if it’s just for a night or two. And that matters, because feeling a bit better, a bit more rested, a bit less sore can be exactly the nudge you need to get back into a broader self-care routine.
It’s not about relying on massage forever. It’s about using it strategically, when you need it, to break the cycle and create the conditions for everything else to fall back into place.
Working With the Right Therapist Makes a Difference
One thing I’d emphasise is not all massage is the same. And who you see, matters. If your pain is muscular in origin - tension headaches, upper back stiffness, shoulder aching from desk posture for example, a well-qualified clinical or sports massage therapist can assess what’s going on, work on the relevant tissues with skill, and give you practical advice alongside the treatment.
Look for someone who is properly qualified (Level 5 or above in the UK), registered with a professional body, and who takes the time to understand your situation before diving in. A therapist who makes you feel heard, explains what they’re doing, and adapts the session to you, rather than delivering a one-size-fits-all routine, is going to get you better results.
What Helps Between Sessions
Massage works best as part of a broader approach, not as the only intervention. If you're in the desk-worker pattern and want to make the most of any treatment you have, a few things are worth building in alongside it.
Movement breaks > The research on prolonged sitting consistently shows that short, frequent movement breaks can help alleviate musculoskeletal discomfort (Waongenngarm, Areerak & Janwantanakul, 2018). Standing up, walking to another room, doing a few shoulder rolls or a gentle neck stretch every 45 to 60 minutes is enough to interrupt the sustained static loading that drives the tension pattern described above.
Slow, deliberate breathing > When you’re stressed or under sustained work pressure, breathing tends to become shallower and faster without you noticing. If that’s the case, try taking a few minutes to breathe slowly and deliberately. This activates the vagus nerve and shifts the nervous system toward parasympathetic dominance. Five minutes, once or twice a day, done consistently over a few weeks has been shown to measurable effects on heart rate variability and baseline stress levels (Laborde et al., 2022)!
Sleep position and pillow height > Worth reviewing if you're waking with neck pain or stiffness. If you are a side sleeper, try making sure you have a thick-enough pillow that it keeps your head in neutral (not tilted toward or away from your shoulder), as this should help reduce overnight load on the cervical muscles.
The Takeaway
If you’re in one of those phases - stressed, sore, not sleeping well, struggling to find time for exercise or self-care - don’t beat yourself up about it. It happens to everyone. If you want a little help, consider booking a massage with a competent therapist you trust, giving you some time to take a breather, reset and relax.
It won’t fix everything. But it might help you feel more like yourself again - and that’s often all you need to start getting back on track.
References
Bervoets, D.C., Luijsterburg, P.A.J., Alessie, J.J.N., Buijs, M.J. & Verhagen, A.P. (2015). Massage therapy has short-term benefits for people with common musculoskeletal disorders compared to no treatment: a systematic review. Journal of Physiotherapy, 61(3), 106–116. [Full text]
Cohen, S.P., Vase, L. & Hooten, W.M. (2021). Chronic pain: an update on burden, best practices, and new advances. The Lancet, 397(10289), 2082–2097. [Full text]
Diego, M.A. & Field, T. (2009). Moderate pressure massage elicits a parasympathetic nervous system response. International Journal of Neuroscience, 119(5), 630–638. [Full text]
Falla, D.L., Jull, G.A. & Hodges, P.W. (2004). Patients with neck pain demonstrate reduced electromyographic activity of the deep cervical flexor muscles during performance of the craniocervical flexion test. Spine, 29(19), 2108–2114. [Full text]
Fuentes, J., Armijo-Olivo, S., Funabashi, M., Miciak, M., Dick, B., Warren, S., Rashiq, S., Magee, D.J. & Gross, D.P. (2014). Enhanced therapeutic alliance modulates pain intensity and muscle pain sensitivity in patients with chronic low back pain: An experimental controlled study. Physical Therapy, 94(4), 477–489. [Full text]
Moseley, G.L. & Butler, D.S. (2015). Fifteen years of explaining pain: The past, present, and future. The Journal of Pain, 16(9), 807–813. [Full text]
Ntoumas, K., Karatzaferi, C., Boubougiatzi, G., Louvaris, Z., Giannaki, C.D., Maridaki, M. & Sakkas, G.K. (2025). Massage positively influences daytime brain activity and reduces arousal state in poor sleepers: A randomised controlled trial. BMC Complementary Medicine and Therapies, 25, 290. [Full text]
Laborde, S., Iskra, M., Zammit, N., Borges, U., You, M., Sevoz-Couche, C. & Dosseville, F. (2022). Effects of voluntary slow breathing on heart rate and heart rate variability: a systematic review and meta-analysis. Neuroscience & Biobehavioral Reviews, 138, 104711.https://doi.org/10.1016/j.neubiorev.2022.104711
Waongenngarm, P., Areerak, K. & Janwantanakul, P. (2018). The effects of breaks on low back pain, discomfort, and work productivity in office workers: a systematic review of randomized and non-randomized controlled trials. Applied Ergonomics, 68, 230–239. https://doi.org/10.1016/j.apergo.2017.12.003